Evidence Base
The MyWay platform patient-facing element has been evaluated through various research studies to ensure it is useful, safe, effective, and delivers benefits.
In summary, the features/ tools have been shown to improve health outcomes and save health services money; through efficiencies, reductions in clinical visits and a reduction in major complications of diabetes.
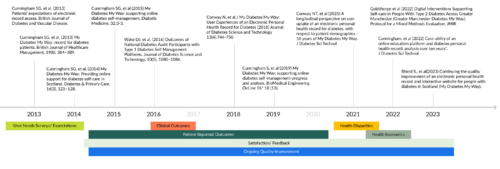
The diagram below summarises key evaluation and design work conducted for the MyWay system up to the beginning of 2025.
Core Product Evaluation
User Centered Design – AI Elements
Structured Education Component

In more detail:
a) Patient Reported Outcomes/ User Satisfaction
Summary findings from an evaluation survey in 2015 of 1,095 users demonstrates that:
The demographics and socioeconomic status of the respondents were in line with the general user base. A further survey published in 2023 demonstrated ongoing general satisfaction and highlighted areas for improvement.
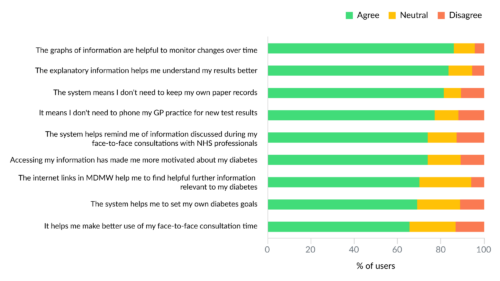
References for above (fig 1) and others that relate to patient-reported outcomes:
- Conway NT et al (2018) My Diabetes My Way: User Experiences of an Electronic Personal Health Record. Jn of Diab Sci and Techn. DOI: 10.1177/1932296818818837
- Shield S. et al (2023) Continuing the quality improvement of an electronic personal health record and interactive website for people with diabetes in Scotland (My Diabetes My Way) Diabetic Medicine DOI: 10.1111/dme.15085
- Cunningham SG et al (2019) My Diabetes My Way: supporting online diabetes self-management – progress and analysis from 2016″ (BMEO-D-17-00369R3) BioMedical Engineering OnLine; 18 (13) DOI: 10.1186/s12938-019-0635-4
- Wake D.J, et al (2016) MyDiabetesMyWay: An Evolving National Data Driven Diabetes Self Management Platform Jn of Diab Sci and Techn;10(5):1050-8. DOI: 10.1177/1932296816648168
- Cunningham SG, et al (2015) My Diabetes My Way: supporting online diabetes self-management. Diabetic Medicine; 32:3-3 DOI: 10.1186/s12938-019-0635-4
- Cunningham SG et al(2014) My Diabetes My Way: Providing online support for diabetes self-care in Scotland Diabetes & Primary Care, 16(3), 123–128[GU1]
- Cunningham SG, et al. (2013) My Diabetes My Way: an electronic personal health record for diabetes. British Journal of Diabetes and Vascular Disease 13(3), 143-49. DOI: 10.1177/1474651413493336– https://diabetesonthenet.com/diabetes-primary-care/my-diabetes-my-way
b) Education Feedback
In addition, we have published results and user feedback from our massive open online courses for patients and carers. These demonstrate excellent feedback/ satisfaction, and self-reported improvements in knowledge and diabetes management. This is illustrated in research conducted in 2020, in which 401 users reported that course satisfaction was high, with the majority reporting that our massive online open course was easy to use and agreeing that it improved their knowledge, motivation, confidence, health and wellbeing, as well as their ability to self-manage their diabetes (see figure belowand first reference).
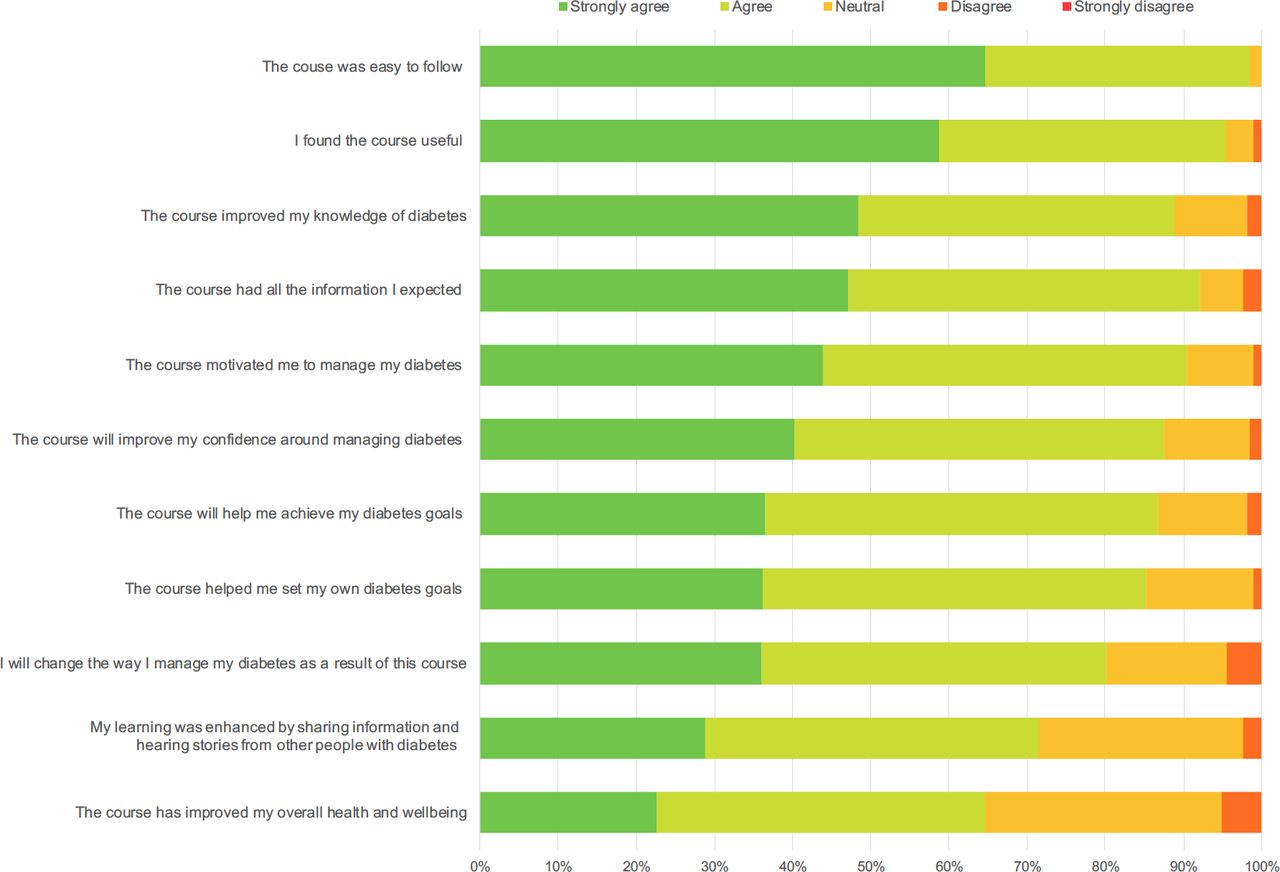
MWDH have demonstrated patient benefits across a number of courses covering different topics as per the publications below:
Reference for above figure* and others:
- *Mackenzie S, Cumming K, Garrell D, Brodie D, Wilson L, Mehar S, Bickerton A, Cunningham SG, Wake DJ (2020) Massive open online course for type 2 diabetes self-management: adapting education in the COVID-19 era. BMJ-Innovations: DOI: 10.1136/bmjinnov-2020-000526
- Mackenzie SC, Cumming KM, Garrell D, Brodie D, Wilson L, Mehar S, Cunningham SG Bickerton A, Wake DJ (2021), Follow-Up of a Massive Open Online Course in Type 2 Diabetes Self-Management Education. J Diabetes Sci Technol.; 15(4):976-977 DOI: 10.1177/1932296821997178
- Mackenzie S C, Wake DJ (2024). Digitising diabetes education for a safer Ramadan: Design, delivery, and evaluation of massive open online courses in Ramadan-focused diabetes education. Primary Care Diabetes; 18(3):340-346 PCD-D-24-00003R1; DOI: 10.1016/j.pcd.2024.03.002
- Mackenzie S C, Cumming K, Mehar S, Wilson L, Cunningham SG, Bickerton A, Wake DJ (2022) Education at Scale: Improvements in Type 1 Diabetes Self-Management Following a Massive Open Online Course (MOOC). Diabetic Medicine 39(8):e14842. DOI: 10.1111/dme.14842
c) Health Outcomes
We have demonstrated improvement in key clinical/ metabolic outcomes through a number of studies in different geographies and using different methodologies including:
1. Observational analysis (from Scotland users up to end September 2015) suggested improvements in key clinical outcomes clinical parameters including HbA1c (n = 2,611), weight (n = 2,297), diastolic BP (n = 2,552), and cholesterol (n = 2026) (all P < .01) 1 year after first login for the patient platform.
Ref: Wake D.J, He J, Czesak A.M., Mughal F, Cunningham, S.G. (2016) My Diabetes My Way: An Evolving National Data Driven Diabetes Self-Management Platform. Journal of Diabetes Science and Technology Aug 22;10(5):1050-8. DOI: 10.1177/1932296816648168
2. A further observational analysis (from Somerset users up to end 2023) indicated significant improvements in key clinical outcomes for people with type 2 diabetes (n = 6457) using the MyWay Diabetes platform in Somerset. Improvements were observed in HbA1c (–8.6 mmol/mol, p < .001), systolic blood pressure (–2.5 mmHg, p < .001), diastolic blood pressure (–2.0 mmHg, p < .001), and triglycerides (–0.1 mmol/L, p = .028) 2 years after registering with MyWay Diabetes.
Ref: Baxter M, Conway N, Bickerton A, Cunningham S.G., MacKenzie S.C., Dickson J, Brodie D, Sainsbury C, Wake D.J. (2025) Impact on diabetes-related health outcomes using a digitally-enabled diabetes self-management platform in Somerset, UK: An interrupted time-series analysis. DOI: 10.1186/s12938-019-0635-4
3. A case control cohort study of Scottish population users versus those in the inactive background diabetes population. This involved 7,689 cohort including 2576 active users with three or more years of follow-up data. The study showed improvements in the following clinical outcomes—HbA1c, hypertension, weight, and lipids—which are discussed further in the cost-effectiveness section. The cohort showed significant improvement in all four outcomes over three years, and these data were used to inform the cost-effectiveness analysis (see further below) Ref: Cunningham, S et al (2023) Cost-utility of an online education platform and diabetes personal health record: analysis over ten years” J Diab Sci and Tech. DOI: 10.1177/19322968211069172
4. NW London cohort data (patient platform branded as Know Diabetes Platform) (unpublished data) Key Points:
- Know Diabetes received high scores on patient-reported usefulness sub-domains related to usability, utility and overall satisfaction.
- The survey respondents reported a high technological literacy level (7.5 out of 10)
- The “good” (14.4) Net Promoter Score suggests a good level of satisfaction and user loyalty among the respondents
- Smartphone (70% of patients) was the most used device to access Know Diabetes, followed by computer/laptop (46% of patients) and tablet (25% of patients).
Clinical Outcomes: The Know Diabetes (KDS) patient records access element has only recently been implemented at scale, therefore there is limited long term data available. Provisional early analysis of initial cohort (using observational data) however looks promising, and further snapshot audits are ongoing.
17987 KDS users’ data were reviewed to assess observational outcomes (comparison of pre and post-data (see methods below)). The platform demonstrated significant improvements/ reductions in HbA1C, BMI, BP, IHD hospital episode admission duration, and GP practice encounters.
c) Short Term Cost Savings
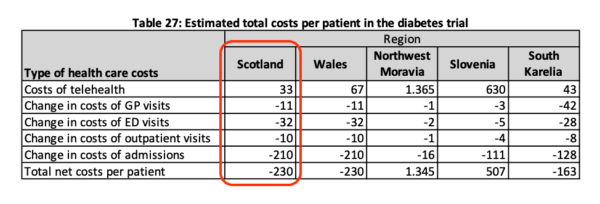
A European funded study using My Diabetes My Way in conjunction with home glucose monitoring upload (through Diasend) was analysed as part of the United4Health Telehealth study as the Model for Diabetes in Scotland. This demonstrated significant cost savings in Scotland of €230 for €33 invested in savings by supporting better personal outcomes and experiences for users through supported self-management and online records access. Savings were derived predominantly from reduced acute admissions as well as through fewer primary, outpatient and emergency department contacts. ** note in table below, other regions used different interventions (not MyWay).
Ref: The National Service Model for Home and Mobile Health Monitoring (HMHM) report (https://tec.scot/wp-content/uploads/2019/08/A-National-Service-Model-for-HMHM-v1.1.pdf).
e) Medium to Longer Term Cost Savings (Health Economics)
Studies conducted by MWDH and independent studies have demonstrated cost-effectiveness. These include:
1. Scotland Cohort Cost-Effectiveness Analysis: Improvements in blood glucose (HbA1c) were modelled to show the likely impact on future events (like heart attacks and strokes) in those with Type 2 diabetes not on insulin. The modelling used the United Kingdom Prospective Diabetes Study (UKPDS) outcomes model which is recognised as a gold standard internationally. The modest costs of the service were more than offset by costs of events avoided over 10 years. The economic study showed both better effect and lower costs and is therefore dominant when compared to usual care alone. From a service investment perspective, the health service will get back about £5 for every £1 spent (outcomes modelled relate to diabetes complications, including cardiovascular outcomes, amputation, blindness, renal failure, mortality and calculated QALYs). For NHS England the estimated return over 10 years using a very conservative approach is £ 337.1m
Ref: Cunningham, S et al (2021) Cost-utility of an online education platform and diabetes personal health record: analysis over ten years” accepted for Journal of Diabetes Science and Technology. DOI: 10.1177/19322968211069172
2. An independent Economic Impact Evaluation Case Study by York Health Economic Consortium, funded by the NHS Innovation Accelerator can be found here.
3. An independent review of the platform was conducted by Health Technology Wales and found to be cost effective with strong recommendation for national commissioning. Report can be found: https://healthtechnology.wales/guidance-published-on-digital-tools-for-diabetes-management
f) User Needs/ User Centred Design
MWDH and partners have conducted various studies to ensure user needs, requirements and feedback are incorporated into design/ product development work. These include:
- Kirkwood JR, Dickson J, Stevens M, Manataki A, Lindsay RS, Wake DJ, Reynolds RM (2024) The User-Centered Design of a Clinical Dashboard and Patient-Facing App for Gestational Diabetes. DOI: 10.1177/19322968241301792
- Jrn Diab Sci Tech (in submission)
- Gardner C., Wake DJ, Halligan J, Brodie D, Silverstein A, Young S, Cunningham S, Sainsbury C, Ilia M, Lucas A, Willis T, Halligan J (2023) Evaluation of prototype risk prediction tools for clinicians and people living with type 2 diabetes in North West London using the think aloud method. Digital Health; DOI: 10.1177/20552076221128677
- Shields C et al. (2022) User-centered design of a novel risk prediction behaviour change tool augmented with an Artificial Intelligence engine (MyDiabetesIQ): A sociotechnical systems approach. JMIR; 8;9(1):e29973 DOI: 10.2196/29973
- Cunningham S G, et al (2013) Patients’ expectations of electronic record access. British Journal of Diabetes and Vascular Disease.
g) MyWay Clinical / AI Work.
In addition, MWHD has worked with partners through a number of funding streams to develop and deploy clinician facing advanced machine learning analytics and decision support.